Limited staffing levels during the pandemic have compromised patient safety, according to striking nurses at several locations around the country. Strikes have also drawn attention to hospital systems that received stimulus funding and posted substantial profits while their staffs faced hazardous workplace conditions, layoffs, and furloughs.
Nurses across the country have organized strikes after the COVID-19 pandemic pushed healthcare workers and systems to their limits. While strikes have been happening at different hospitals and through several unions, one message has stood out most: nurse staff levels are not adequate for proper patient care.
Research has shown that patient care suffers when nurses have to care for too many patients at one time. It has also shown that proper nurse staffing levels can reduce in-hospital deaths and other adverse patient outcomes. There are currently no federal mandates that regulate the ratio of registered nurses to patients.
California is the only state that has a nurse-to-patient ratio statute. Even with this mandatory ratio, the law was temporarily waived by Governor Gavin Newsom (D) when COVID-19 surges overwhelmed hospitals in 2020.
Many nurses in the state protested the use of waivers and argued that waiving the strict minimums contributed to other staffing problems, like canceling traveling nurse contracts and laying off and furloughing nurses. Despite the drastic healthcare demands of the pandemic, many California hospitals laid off or furloughed nurses and medical personnel, citing loss of revenue. In February 2021, California halted the approval of staffing waivers, a decision that was celebrated by the California Nurses Association.
While state laws in California make the situation there somewhat unique, it is nevertheless a prime example of the need to balance legal oversight, hospital profits and budgets, and nurses’ firsthand experiences in the pursuit of proper healthcare guidance. Nurses on strike are seeking specific solutions with their employers and hospitals, but their collective message has brought renewed national attention to nurse-to-patient care levels and its effect on the quality of overall healthcare.
Strikes Across the Country
Strikes have been organized by nurses’ unions across several states, including Massachusetts, Pennsylvania, and California.
Nurses at St. Vincent Hospital in Worcester, Massachusetts have been on strike since March 8. At almost four months, it has become the longest nurses’ strike in 30 years. The hospital is a subsidiary of Tenet Healthcare, a public company that owns 65 hospitals and approximately 450 other medical centers across the country.
The nurses on strike are part of the Massachusetts Nurses Association (MNA), a union that St. Vincent nurses joined 20 years ago to protest low staffing levels. Nurses say that the current 1:5 ratio of nurse to patients is unsafe. As part of their demands, nurses are advocating for a 1:4 ratio on medical and surgical floors and telemetry units, and increased staffing in the emergency department. After proposals from both sides were counter-offered and refused, 90% of union-represented nurses who cast a ballot on February 10 were in favor of striking.
The MNA has been involved in patient and nurse staff safety since the start of the pandemic. In April 2020, they announced that they had acquired needed PPE for nurses with support from other organizations. In particular, they noted that a generous donation of $150,000 from Massachusetts-based drug development companies helped fund the purchase of KN95 masks and face shields. The union also sparred with Tenet management last May when the hospital rolled out voluntary furloughs for nurses. The union sought to protect nurses from understaffed COVID-19 units, which were being reported by nurses on the job. These factors contributed to the nurses’ strike 11 months later.
Other strikes have been, on average, a few days long. In April 2021 at Tyler Memorial Hospital in Tunkhannock, Pennsylvania, nurses and hospital staff staged a three-day strike and returned to work after picketing for safe staffing levels. While the strike is over, contract negotiations with the hospital are still ongoing. The hospital is part of Commonwealth Health System, which is owned by Community Health Systems, a competitor of Tenet Healthcare.
Another April strike at Barton Memorial Hospital in South Lake Tahoe, California concluded after two days. The strike included 155 unionized nurses represented by the California Nurses Association. Barton Memorial Hospital is a part of Barton Health, a community-based healthcare nonprofit. The hospital is the only one in the South Lake Tahoe area.
The reasons for striking included staffing level concerns and increasing nurse turnover rates, which affect patient safety. According to the hospital, Barton’s turnover rate has increased from 9.5% in 2016 to 13.7% in 2020.
Barton Memorial responded to the strike by stating that a contract had been proposed in February with a 17% average pay increase over four years. Failed contract negotiations had led to a similar one-day strike in 2019. Negotiations in 2021 are still ongoing.
Some strikes have been avoided altogether by last-minute agreements. In Connecticut, a planned strike at 33 nursing facilities in May was postponed after the administration of Governor Ned Lamont (D) reached an agreement with union leaders to provide $267 million in state funding for wage increases for nursing home staff. The new funding will increase minimum wages to $20 per hour for certified nursing assistants and $30 per hour for licensed practical nurses.
Governor Lamont’s administration similarly reached a deal with unionized group home workers following the agreement of the nursing home workers’ contract. The ‘11th hour’ deal averted a planned strike at 12 picketing locations throughout the state. The group home workers numbered about 2,000 staffers, including support staff, program coordinators, and licensed practical nurses.
Nurses’ decisions to go on strike is the result of strained or failed contract negotiations with employers. Many of the strikes are rooted in issues that prompted work stoppages over the past few years.
Should Nurse-Patient Ratios Be Mandated?
The debate over mandated nurse staffing ratios is not a new one, especially when it comes to disputes over research and data.
Healthcare systems and organizations that represent such healthcare providers, such as the Illinois Health and Hospital Association, tend to oppose staffing ratios and have argued that there is not enough conclusive evidence that mandated ratios have a positive impact on quality of care.
Opponents of mandated ratios have also argued that mandates would drive up staffing costs and overall operating expenses. In Illinois, opponents of a proposed nurse staffing mandate bill, called the Safe Patient Limits Act, objected to the proposed fine of $25,000 a day for hospitals in noncompliance with staffing numbers. In 2021, the Safe Patient Limits Act was adjourned indefinitely by Illinois lawmakers.
The American Nurses Association (ANA), which represents 4 million nurses across the country, has taken a surprisingly moderate stance. The organization has supported flexibility when determining proper staff levels, such as assigning nurse ratios based on level of required care per patient versus a mandatory minimum per patient. “It’s not that we’re against ratios,” Janet Haebler, a senior associate director for ANA told WHYY. “We’re against legislating ratios.”
While the ANA’s approach may not endorse number-based mandates, it does support a staffing plan that puts nurses in charge of ultimate decision-making. The organization’s staffing principles give nurses a full and equal role as members of the care team and recommend that nurse-specific and patient-specific factors be considered, such as a nurses’ years of experience and their patient acuity.
The numerous strikes for staff ratios and patient safety seem to indicate that nurses themselves overwhelmingly support some kind of minimum standard. As workers with direct experience in the field, nurses are oftentimes eyewitnesses to preventable system failures.
NursesTakeDC, a nonprofit that advocates for safe nurse staffing, is currently conducting a survey for nurses to report their staff levels and to indicate if they were getting their breaks. Of the current 733 respondents, 76% have reported unsafe staffing and 65% reported not receiving their break.
Stimulus Payments, Profits Raise Questions About Hospital Choices
Organized strikes and the financial impact of the COVID-19 pandemic have brought increased scrutiny to hospital profits and spending, especially as many healthcare providers received significant amounts of cash from the federal government’s pandemic relief efforts.
During the fourth week of the St. Vincent Hospital strike, the City of Worcester confirmed that Tenet Healthcare had spent over $22 million on replacement nurses and security details. The MNA calculated that the funds used for security alone could have addressed many of the key issues that had prompted the nurses to strike.
In addition, many hospitals furloughed or laid off their healthcare workers during surges of the COVID-19 pandemic, raising questions over the use of stimulus funding and the and the companies’ deep cash reserves.
Doris Carroll, a nurse who helped launch NursesTakeDC, told WHYY: “[Nurses] became a line item in the budget that costs the hospital money. Who is the largest labor force in the hospital? It’s nurses. And if hospital administrations can still make a profit and do it with a skeleton crew of nurses, they will do it anytime.”
Tenet Healthcare, for example, reported $3.1 billion of available cash on hand during the second quarter of 2020. Yet, it still furloughed approximately 11,000 workers last year, citing a decline in elective surgeries and other procedures that contribute heavily to its revenue. Several executives at Tenet took pay cuts and CEO Ron Rittenmeyer donated an estimated $375,000 of his own salary to a fund to assist furloughed workers. Mr. Rittenmeyer’s 2020 compensation, which includes stock awards and bonuses, still totaled $16.68 million.
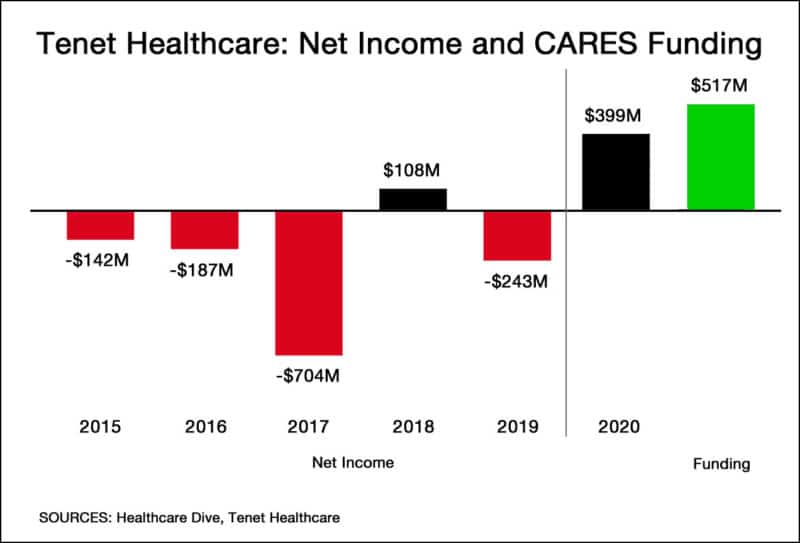
Tenet, along with other major for-profit healthcare providers like Community Health Systems (CHS), received grant money from the $175 billion targeted to providers by the CARES Act and the Paycheck Protection Program and Health Care Enhancement Act. The money does not have to be repaid. Tenet received $517 million in CARES funding alone, while CHS was granted $420 million.
Despite the pandemic, Tenet posted a $399 million profit in 2020, its most profitable year – and only its second profitable year – in the last six years. Similarly, CHS posted a profit of $511 million – its first profitable year since 2015.
The distribution of relief funds to these and other companies has raised questions about their decision-making and has illuminated areas of unequal distribution. A Kaiser Family Foundation study found that when the Department of Health and Human Services (HHS) began distributing grants to hospitals from the $175 billion allocated by the two relief bills, the funding was not evenly reaching hospitals that served low-income patients. The study suggested that the distribution formula used by HHS favored hospitals that had a larger share of private insurance reimbursement, further exacerbating the problem of access to healthcare during a time of crisis.
What’s Next?
Reports of nurses striking across the nation may be what the movement needs to garner attention and public support for improving and sustaining access to quality patient care. How staff ratios should be determined, how much nursing care should cost, and how it should be legislated, will all play a role in the future of quality healthcare.
And, for the time being, St. Vincent Hospital nurses are continuing their pursuit of patient safety on behalf of their hospital and the industry. “People need to start demanding,” Marie Ritacco, registered nurse and vice president of the MNA, told The Nation. “This is for the good of our communities, and we deserve this. This is our money from the CARES Act and the Recovery Act getting filtered into these institutions, and we need to demand better. And so taking on the fight is definitely a labor of love.”
Problem Addressed: Access to Healthcare
Written by Anna Luo
Published on June 19, 2021
Feature image: Photo by Boyloso
Sources
National Nurses United, “National Campaign for Safe RN-to-Patient Staffing Ratios”, https://www.nationalnursesunited.org/ratios, accessed Jun 1, 2021
Rebecca A. Paulsen, “Taking nurse staffing research to the unit level”, NCBI, Jun 11, 2018, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6039374/, accessed Jun 1, 2021
National Nurses United, “Nurse Staffing Standards for Hospital Patient Safety and Quality Care Act”, https://www.nationalnursesunited.org/sites/default/files/nnu/documents/0421_Ratios_Federal_FactSheet.pdf, accessed Jun 1, 2021
National Nurses United, “What does the California Ratios Law Actually Require?”, https://www.nationalnursesunited.org/what-does-california-ratios-law-actually-require, accessed Jun 1, 2021
Olga R. Rodriguez, “California bypasses tough nurse care rules amid virus surge”, Associated Press, Jan 8, 2021, https://apnews.com/article/california-coronavirus-pandemic-f5d228109141806f2da4b6f03f985b16, accessed Jun 1, 2021
National Nurses United, “California nurses declare victory as state tells hospitals all waivers of safe staffing standards expire by Feb. 8”, Feb 1, 2021, https://www.nationalnursesunited.org/press/california-nurses-declare-victory-safe-staffing-standards, accessed Jun 1, 2021
Jill Castellano, “California hospitals given leeway to use ‘last resort’ staffing waivers, analysis shows”, CBS 8, Mar 4, 2021, https://www.cbs8.com/article/news/local/inewsource/california-hospitals-given-leeway-using-last-resort-staffing-waivers-analysis-shows/509-24117ce4-6cc6-4536-9c66-622dacc5fda7, accessed Jun 1, 2021
Andie Judson and Victor Nieto, “California hospitals lacking non-COVID patients laying off staff amid pandemic”, ABC 10, May 11, 2020, https://www.abc10.com/article/news/health/coronavirus/california-hospitals-laying-off-staff-amid-coronavirus-pandemic/103-fbfdaad6-4d43-4a9f-b458-ad0afac79c5f, accessed Jun 1, 2021
Sarah Jaffe and C.M. Lewis, “Nurses Are Striking Across the Country Over Patient Safety”, The Nation, May 6, 2021, https://www.thenation.com/article/activism/nursing-strike-massachusetts-covid/, accessed Jun 1, 2021
Nora De La Cour, “Union Nurses in Massachusetts Are Waging the Longest Current Strike in the US”, Jacobin Mag, May 11, 2021, https://www.jacobinmag.com/2021/05/union-nurses-saint-vincent-strike-massachusetts-tenet-mna, accessed Jun 1, 2021
Tenet Healthcare, “Who We Are”, https://www.tenethealth.com/about, accessed Jun 10, 2021
Cyrus Moulton, “What you need to know about the St. Vincent strike”, Telegram & Gazette, Jun 2, 2021, https://www.telegram.com/story/news/2021/06/02/what-you-need-know-st-vincent-hospital-strike-massachusetts-nurses-association-and-tenet-healthcare/7504960002/, accessed Jun 2, 2021
PR Newswire, “With Help from Generous Donor, MNA Purchases and Begins to Distribute Tens of Thousands of Desperately Needed KN95 Respirator Masks to Its Nurses and Healthcare Professionals Across the State”, Apr 15, 2020, https://www.prnewswire.com/news-releases/with-help-from-generous-donor-mna-purchases-and-begins-to-distribute-tens-of-thousands-of-desperately-needed-kn95-respirator-masks-to-its-nurses-and-healthcare-professionals-across-the-state-301040877.html, accessed Jun 1, 2021
Danielle Ray, “Nurses, St. Vincent Hopsital administration clash over furloughs”, Telegram & Gazette, May 1, 2020, https://www.telegram.com/news/20200501/nurses-st-vincent-hospital-administration-clash-over-furloughs, accessed Jun 1, 2021
PA Homepage, “Tyler Memorial workers return to work after a 3-day strike”, Apr 24, 2021, https://www.pahomepage.com/top-news/tyler-memorial-workers-return-to-work-after-a-3-day-strike/, accessed Jun 1, 2021
Commonwealth Health, “About Us”, https://www.commonwealthhealth.net/hospital-about-us, accessed Jun 1, 2021
Kelly Gooch, “Barton Memorial Hospital nurses strike: 6 things to know”, Beckers Hospital Review, Apr 16, 2021, https://www.beckershospitalreview.com/hr/barton-memorial-hospital-nurses-strike-6-things-to-know.html#:~:text=About%20155%20union%2Drepresented%20nurses,began%20negotiations%20in%20March%202018, accessed Jun 1, 2021
Barton Health, “Union Facts”, https://www.bartonhealth.org/tahoe/union-facts.aspx, accessed Jun 1, 2021
KCRA, “Tahoe nurses strike outside Barton Memorial Hospital”, Apr 17, 2021, https://www.kcra.com/article/tahoe-nurses-strike-outside-barton-memorial-hospital/36152590, accessed Jun 1, 2021
Susan Haigh, “Connecticut nursing home workers postpone planned strikes”, Associated Press, May 13, 2021, https://apnews.com/article/business-nursing-homes-government-and-politics-health-d430b42100c1f973081e942aada0f2a8, accessed Jun 1, 2021
Daniela Altimari, “Strike averted for 2,000 Connecticut group home workers after an 11th-hour deal on wages and beenfits is reached”, Hartford Courant, Jun 3, 2021, https://www.courant.com/politics/hc-pol-group-home-strike-friday-20210603-aedo32aizvcd5nb3ela2f5hl7a-story.html, accessed Jun 5, 2021
Illinois Health and Hospital Association, “State Position Paper: IHA Opposes Mandatory Nurse Staffing Ratios”, https://www.team-iha.org/files/non-gated/advocacy/oppose-hb3585-factsheet.pdf, accessed Jun 1, 2021
Liz Tung, “Why mandated nurse-to-patient ratios have become one of the most controversial ideas in health care”, WHYY, Nov 29, 2019, https://whyy.org/segments/why-mandated-nurse-to-patient-ratios-have-become-one-of-the-most-controversial-ideas-in-health-care/, accessed Jun 1, 2021
Tony Abraham, “Fight for mandated nurse-to-patient ratios heats up”, Healthcare Dive, Jun 15, 2018, https://www.healthcaredive.com/news/fight-for-mandated-nurse-to-patient-ratios-heats-up/525225/, accessed Jun 5, 2021
Illinois General Assembly, “Bill Status of HB2604”, https://ilga.gov/legislation/BillStatus.asp?DocNum=2604&GAID=15&DocTypeID=HB&LegID=118738&SessionID=108&SpecSess=&Session=&GA=101, accessed Jun 1, 2021
Chaunie Brusie, “ANA Updates Nurse Staffing Guidelines To Support Flexibility”, nurse.org, Dec 4, 2019, https://nurse.org/articles/nurse-staffing-ana-guidelines/#:~:text=The%20organization%20believes%20that%20a,such%20as%20acuity%20and%20intensity, accessed Jun 1, 2021
NursesTakeDC, “Report Your Current Staffing”, https://www.nursestakedc.com/report-your-current-staffing, accessed Jun 1, 2021
Jessica Silver-Greenberg, Jesse Drucker, and David Enrich, “Hospitals Got Bailouts and Furloughed Thousands While Paying C.E.O.s Millions”, New York Times, Jun 8, 2020, https://www.nytimes.com/2020/06/08/business/hospitals-bailouts-ceo-pay.html, accessed Jun 1, 2021
PR Newswire, “Dallas-Based Tenet Healthcare Spending Over $22 million to Prolong St. Vincent Nurses Strike Fourth Week to Avoid Staffing Improvements to End Patient Safety Crisis”, Mar 29, 2021, https://www.prnewswire.com/news-releases/dallas-based-tenet-healthcare-spending-over-22-million-to-prolong-st-vincent-nurses-strike-for-fourth-week-to-avoid-staffing-improvements-to-end-patient-safety-crisis-301257447.html, accessed Jun 1, 2021
Press Release, “Tenet Reports Results for the Second Quarter Ended June 30, 2020 and Provides Update on Effects of COVID-19”, Businesswire, Aug 30, 2020, https://www.businesswire.com/news/home/20200803005737/en/Tenet-Reports-Results-for-the-Second-Quarter-Ended-June-30-2020-and-Provides-Update-on-Effects-of-COVID-19, accessed Jun 5, 2021
Alia Paavola, “Tenet furloughs 10% of staff; CEO donates to employee fund”, Beckers Hospital Review, Apr 18, 2020, https://www.beckershospitalreview.com/finance/tenet-furloughs-10-of-staff-ceo-donates-to-employee-fund.html, accessed Jun 1, 2021
Jack O’Brien, “Tenet CEO: Cares Act Provided ‘Reasonable, But Not Complete Relief’”, HealthLeaders, Aug 3, 2020, https://www.healthleadersmedia.com/finance/tenet-ceo-cares-act-provided-reasonable-not-complete-relief, accessed Jun 1, 2021
Samantha Liss, “Here’s how much for-profit hospitals have received in bailout funding so far”, Healthcare Dive, May 26, 2020, https://www.healthcaredive.com/news/heres-how-much-for-profit-hospitals-have-received-in-covid-19-bailout-fund/578378/, accessed Jun 1, 2021
Ayla Ellison, “Tenet CEO’s compensation drops by $7.6M”, Becker’s Hospital Review, Mar 29, 2021, https://www.beckershospitalreview.com/compensation-issues/tenet-ceo-s-compensation-drops-by-7-6m.html#:~:text=Though%20some%20top%20executives%20at,to%20Tenet%27s%20shareholder%20proxy%20statement, accessed Jun 1, 2021
Press release, “Tenet Reports Fourth Quarter 2020 Results; Announces Plan to Retire $478 million of Debt; Provides 2021 Financial Guidance”, Tenet Healthcare, Feb 9, 2021, https://investor.tenethealth.com/press-releases/press-release-details/2021/Tenet-Reports-Fourth-Quarter-2020-Results-Announces-Plan-to-Retire-478-million-of-Debt-Provides-2021-Financial-Guidance/default.aspx, accessed Jun 10, 2021
Press release, “Community Health Systems, Inc. Announces Fourth Quarter and Year Ended December 31, 2020 Results and 2021 Guidance”, Businesswire, Feb 17, 2021, https://www.businesswire.com/news/home/20210217005954/en/Community-Health-Systems-Inc.-Announces-Fourth-Quarter-and-Year-Ended-December-31-2020-Results-and-2021-Guidance, accessed Jun 10, 2021
Karyn Schwartz and Anthony Damico, “Distribution of CARES Act Funding Among Hospitals”, Kaiser Family Foundation, May 13, 2020, https://www.kff.org/health-costs/issue-brief/distribution-of-cares-act-funding-among-hospitals/, accessed Jun 1, 2021
Have a Suggestion?
Know a leader? Progress story? Cool tool? Want us to cover a new problem?