Key Takeaways
- The US spends more per person on healthcare than other wealthy countries but trails behind them in key health indicators like lower life expectancy.
- Access to healthcare in the US is limited by high cost, lack of insurance coverage, and a shortage of healthcare providers.
- Efforts to resolve these problems are deeply polarizing and typically provoke powerful industry interests that stand in the way of expanding access.
- The complex marketplace for healthcare services doesn’t always incentivize better care for more people.
The US is the wealthiest country in the world but it trails behind other wealthy countries in key health indicators, like life expectancy. Over the last four decades, life expectancy in the US has risen significantly more slowly than in other high-income countries, and in recent years, it has virtually stopped rising.
Yet, we spent $10,966 per person on healthcare in 2019, nearly twice the average of comparable countries.
At the same time, many Americans lack access to affordable healthcare. 80% of rural patients live in counties labeled by the federal government as “medically underserved.” Tens of millions are uninsured; tens of millions more are underinsured and can’t afford out-of-pocket medical costs.
Why is it that we spend so much on healthcare when so many of us lack reasonable access? A primary reason is that the American healthcare system is a complex hodge-podge of government insurance, private insurance, and government-owned institutions (such as the Veterans Administration). Or, as healthcare policy expert Simon F. Haeder called it, a “patchwork that nobody likes.”
Our convoluted system doesn’t limit access per se. Rather, it often creates perverse incentives for actors within the system to limit access. Hospitals that don’t turn a profit are closed, sometimes leaving neighboring communities without vital resources in direct contradiction to the “do no harm” ethic that is a driver of medical practice. Hospitals and pharmaceutical companies charge what insurance companies will pay, not what patients can afford. The complex requirements of the private insurance industry place an administrative burden on healthcare providers, inflating overall costs to a point that threatens the financial health of many patients.
This state of affairs stands, once again, in marked contrast to other wealthy countries. Every modern industrialized country except the United States has come to treat healthcare as a right guaranteed by the government. These nations deliver universal healthcare to their citizens through a variety of methods, from government-owned healthcare facilities to highly regulated compulsory insurance. The UK, for instance, provides fully-nationalized, free-at-point-of-use healthcare for everyone.
The US has failed to fully embrace the view of healthcare as a right for several reasons: hyperpartisan politics, industry interests, and a lack of immediate contact with the healthcare system. The result has been a lack of commitment to healthcare reform.
The most recent comprehensive effort at reform was the Patient Protection and Affordable Care Act of 2010 (ACA, also known as the Affordable Care Act and Obamacare). Its main goals were to expand health insurance coverage to more consumers, provide more consumer protection, improve the quality of care, and control costs.
In 2009, 4,525 lobbyists — eight for each member of Congress — worked to influence health reform bills. Ultimately, the ACA passed without a single Republican vote. In the decade after its passage, the number of insured Americans increased, but so did cost.
More recently, the COVID-19 crisis further stressed a struggling system. But it also revealed opportunities as, for example, more Americans than ever are receiving care via online video calls, a form of medical practice known as telehealth.
As costs continue to rise and hospitals continue to close, we will need to address these barriers to healthcare access.
Problem Definition
Three broad challenges stand out in the American healthcare system as they relate to access to healthcare:
Lack of insurance
Tens of millions of Americans lack healthcare insurance or are underinsured, meaning their out-of-pocket healthcare costs or their plan deductibles took up at least 5% of their annual incomes. Lack of adequate coverage limits access to needed healthcare, as many who lack sufficient insurance will face severe financial hardship if they seek treatment for a serious illness.
Soaring costs
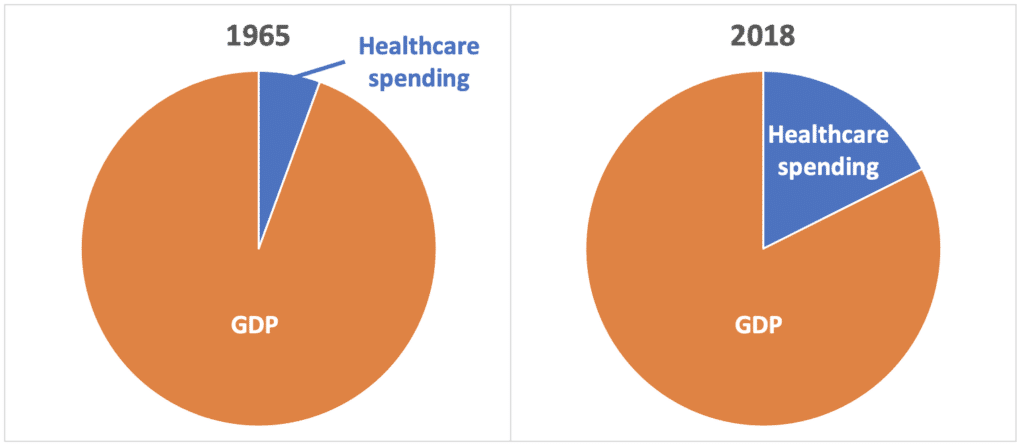
The US pays more per person for healthcare than other industrialized countries, but trails in most indicators of population health. Healthcare spending now accounts for 17% of our economy. Plus, rising costs crowd out other social needs and priorities.
Shortage of providers
Many patients experience difficulty finding care because of healthcare provider and facility shortages. While a factor in some urban communities, this problem is worse in rural America.
Problem Scope
Millions un- and under-insured
By the middle of the last century, as the cost of medical care started to rise, access to care required some form of health insurance. Most Americans who had health insurance at that time received it as a benefit provided by their employers. Retired people, unemployed people, and poor people, however, did not have insurance. Only after Congress expanded Social Security and established the Medicare and Medicaid programs did millions of Americans, and particularly the elderly, who lived at or near poverty levels, have access to insurance, and so, to medical care.
Even so, in 2009 (one year prior to passage of the Affordable Care Act), more than 46 million Americans reported being without health insurance. Following the establishment of the Affordable Care Act (ACA), and despite committed opposition to limiting its impact, the number of Americans without insurance fell to 27.8 million by 2018.
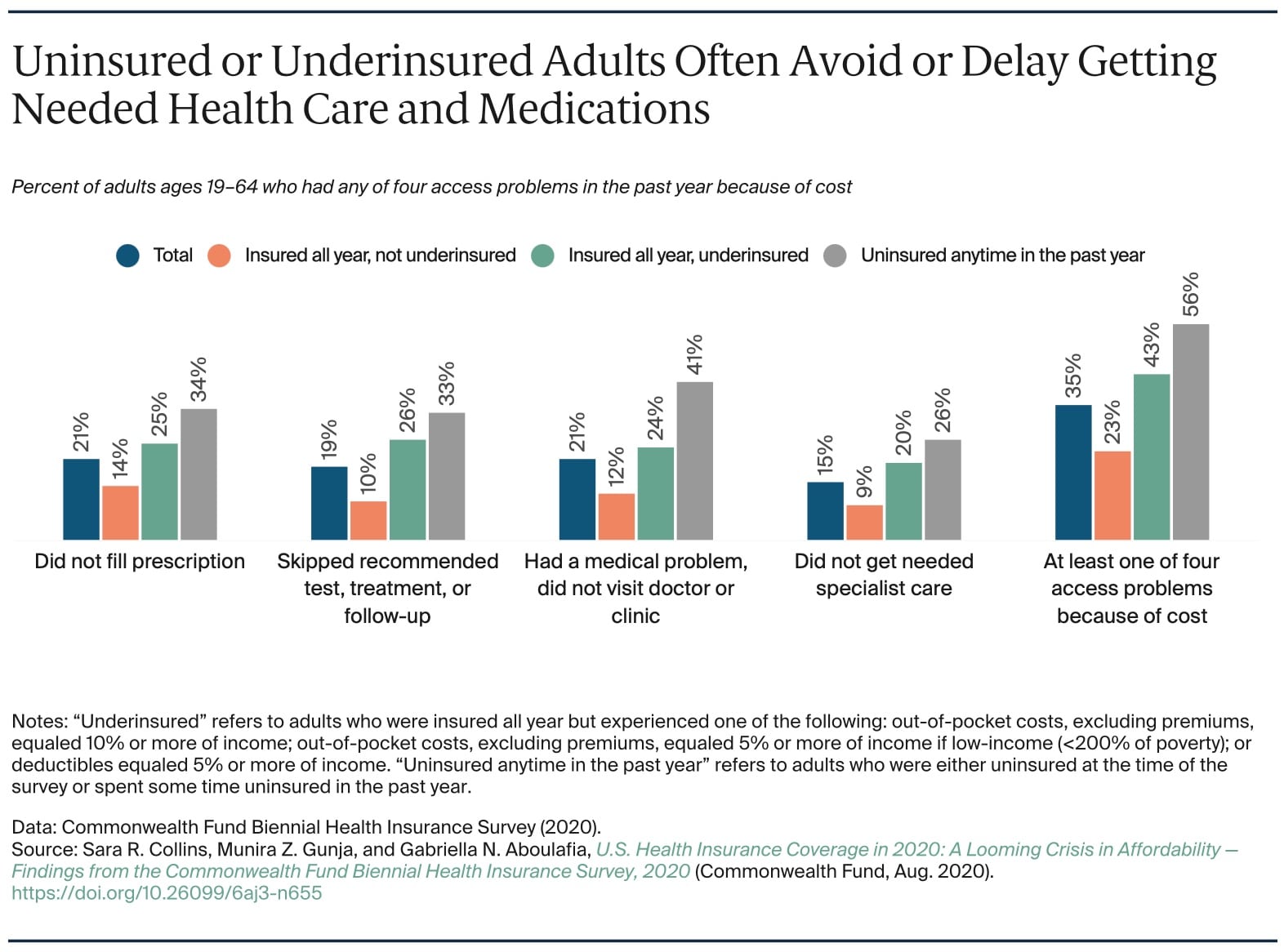
Still, 12.5% of Americans were uninsured for the entirety of 2020. Over 1 in 5 were underinsured, with high-deductible plans and high out-of-pocket costs. According to a Gallup poll released in December 2019, one-third of American families put off seeking medical care because they were concerned about costs. The Gallup results are consistent with an earlier study by the American Cancer Society, which found that 56% of American adults reported experiencing some form of financial hardship related to seeking medical care, be it affordability, stress, or delaying care due to cost.
Rising costs
Healthcare costs have increased at rates well ahead of inflation for decades. According to the US Centers for Medicare and Medicaid Services (CMS), US healthcare spending as a percentage of GDP grew from 5.6% in 1965 to 17.7% in 2018. Research from The Commonwealth Fund indicates that, in 2016-17, 23.6 million Americans with employer-provided insurance spent at least 10% of their income on either their share of the insurance premium or out-of-pocket costs. The Commonwealth Fund defines this as a high contribution relative to income.
Furthermore, spending in the US is well out of step with other wealthy countries. The US spent $10,966 per person on healthcare in 2019, nearly double the median of other high-income countries. Switzerland, the country that is second on the list, spends around $7,500.
Yet, despite the higher spending, health outcomes in the US are worse than outcomes in these other countries. To name a few examples, the US has the highest infant mortality rate of any high-income country and ranks poorly on premature birth rates and the proportion of children who live to age 5, according to the US National Research Council. Life expectancy is nearly three years lower than the average of other comparable countries, and has actually declined in recent years.
A study by the Commonwealth Fund ranked the US system 11th of 11 high-income countries in overall healthcare system performance (compared with countries such as Australia, Canada, France, Germany, and Norway).
With no end in sight to the rise of healthcare costs, there is a fear that healthcare could become even more unaffordable. What is driving these costs?
High administrative costs
The US spends 8% of total national health expenditures on administration, compared with an average of 3% among all high-income countries, as measured by the Commonwealth Fund.
Researchers lay the difference largely at the feet of a cumbersome private insurance industry. Contrary to common belief that the private sector is more efficient than the government, these administrative costs do not occur with the federal government’s Medicare program. Studies that peg private insurance administrative costs at up to 17% find that Medicare’s administrative costs are only 2%.
High administrative costs related to the private insurance industry stem from overhead costs, including sales, marketing, billing, and advertising, and providers’ costs for claims submissions, claims reconciliation, and payment processing.
Drug spending
Annual per-capita, or per person, spending on drugs is $1,443 in the US, compared with a range from $466 to $939 in similar countries.
One factor contributing to this difference is that pharmaceutical companies regularly charge much more for the same drugs in the US than they do in other countries. Other countries do not allow pharmaceutical companies to set their own prices, using a variety of approaches to control them.
In the US, companies are generally free to charge what they will. Insurers often negotiate prices. However, the largest health insurer in America—Medicare—is forbidden by law from negotiating lower drugs prices with pharmaceutical companies.
A free market? In the United States, federal law prohibits the largest health insurer in the country – Medicare – from negotiating with pharmaceutical companies for lower drug prices.
Labor costs
Physicians’ salaries are high in the US. The average salary for an American general practitioner is $218,173, which is nearly twice the average in other wealthy countries. Some specialists earn more than $400,000 and several are near or over the $500,000 threshold. Prior to the pandemic, cash compensation for physicians had increased steadily over the last decade.
There are a number of explanations for why this is the case, including the high cost of medical school and subsequent student debt, and restrictions on the number of people who are accepted into the country’s residency system. Whatever the reason, however, the bottom line remains: High salaries mean high cost of care.
Lack of competition
Healthcare organizations have been swept up in a wave of consolidation in recent years. The merging entities often say that economies of scale will allow lower prices. But there is evidence that a stronger force—a lack of competition—leads to higher prices.
Because they serve so many patients, large-scale healthcare providers are able to dictate what prices they will charge to the insurers. In Southern California, according to a study of its own employees by Kaiser Health News, insurer Cigna paid a large hospital chain, Sutter Health, nearly double what it paid an independent primary-care doctor for the same vaccination.
Lack of Patient Input on Price
Despite the “consumerization” of healthcare and the resulting language asserting that patients are “healthcare consumers”, it’s not you, the patient, that is negotiating the cost of your care. Nor, if your employer is contracting with your insurer, is your employer. Instead, insurers and healthcare providers – primarily large hospital systems and networks of care – are generally the only two constituencies who have a say in pricing, and their incentives are not necessarily aligned with cost control.
According to The Health Care Blog, “[H]ealth insurers … have little to no incentive to hold down the price of care. Rather, they directly benefit when the price of care rises.” That’s because for many health insurers, employer-provided insurance represents a majority of their business, and the insurers earn a set administrative fee regardless of the medical costs incurred.
In 2018, ProPublica and NPR began reporting on the relationship between health insurers and the healthcare industry. What they found was no surprise: pricing for medical procedures is not transparent to patients or their employers who contract with the insurers. And those prices might sometimes be three times what Medicare pays for the same procedures. According to a report in the NPR-ProPublica series, one healthcare provider in New York billed a patient’s insurer the negotiated in-network rate of $70,000 for a partial hip replacement; the insurer paid 90%, or $63,000, and the patient paid the rest. Medicare, on the other hand, had negotiated a rate of just over $20,000 for the same procedure; FAIR Health, a nonprofit committed to increasing transparency in medical pricing, estimated the total in-network price of the surgery at $29,162.
Yet, the patient’s portion of the $70,000 bill was 10%, meaning he had to pay $7,000, not the $2,916 that the FAIR Health estimate would have required.
A look at just one line item in the bill is revealing: the ball joint that was implanted in the patient during the surgery would have cost the provider $1,500. Yet, the provider charged the insurer the in-network rate of $26,068.
An Employer Strikes Back
The ProPublica-NPR series also reported the story of how Montana’s Department of Administration, led by Marilyn Bartlett, changed the game. As the employer of 30,000 Montanans, the Department did what few other employers have done: it directly entered negotiations with the healthcare providers in the state and set ground rules for using reference-based pricing that would determine which providers the state’s benefit plan – covering 30,000 “healthcare consumers” – would include.
An independent analysis estimates the state has saved $47 million in its first two years since making the transition to reference-based pricing, a method that limits pricing to an agreed-upon multiple of the Medicare price schedule. Montana currently pays between 220% and 250% of Medicare rates, whereas it previously paid as much as 611%.
Shortage of Healthcare Providers
In many parts of the country, regardless of their ability to pay, patients have difficulty gaining access to healthcare because of a shortage of providers. This problem is especially acute in rural areas.
As noted in the Washington Post, “The federal government now designates nearly 80% of rural America as ‘medically underserved’.” Almost 20% of the US population lives in rural areas, but fewer than 10% of physicians practice in them.
The gap between rural and urban access is only getting worse. A July 2019 New England Journal of Medicine article predicted that the number of physicians practicing in rural areas will fall by almost 23% by 2030. Many workforce studies predict shortages of physicians in both primary care and specialties in coming years because not enough physicians are being trained. And since 2010, 106 rural hospitals have closed and nearly 200 are on the verge of collapse.
Contributing to this trend of hospital closures are the lower rates of insurance among the rural population. By law, hospitals are required to treat and stabilize patients who appear at their emergency departments, regardless of the patients’ ability to pay. In hospitals where patient volumes are at a more sustainable level, those patients who are able to pay for services – generally through their insurance provider – are also subsidizing the cost of serving the uninsured. The low volume of insured patients in rural hospitals prevents the hospitals from following that model.
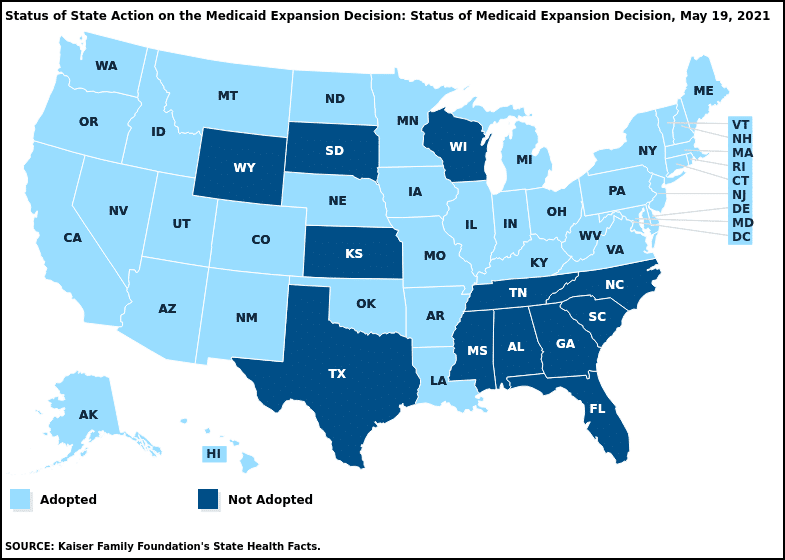
The ACA addressed this problem by giving states the opportunity to expand coverage through Medicaid. Medicaid expansion would allow hospitals to bill the public insurance program for services provided to uninsured patients. To date, however, 12 states have chosen not to adopt Medicaid expansion – and 73% of recent hospital closures occurred in those states.
At the same time, adults living in rural areas report poorer health status with higher rates of major chronic conditions, higher rates of alcohol and opioid abuse, and lower rates of health insurance coverage compared with those living in metropolitan areas. Not surprisingly, life expectancy has also fallen behind in rural areas.
Limits to What We Know
ACA’s Impact on Provider Shortage
One concern regarding the ACA’s goal of expanding healthcare coverage was that, given the existing shortage of healthcare providers, the medical infrastructure would not be able to absorb the influx of new patients. Although the ACA greatly increased the number of people with insurance, especially through Medicaid, “findings on expansion’s effect on provider capacity are mixed, with studies showing increases, decreases, or no effects on measures like appointment availability or wait times”, according to a report by Kaiser Health News.
The Best Alternative to Fee-for-Service
The American system is primarily based on a fee-for-service model, in which healthcare providers are paid for each service they provide. Critics note that this system rewards providers for treating illnesses, instead of for keeping people healthy, and provides incentives for incurring more costs. There is a built-in incentive to do more (and more expensive) tests and more treatment, because the more one does, the more one gets paid. This approach can encourage wasteful use of resources by having different providers focused narrowly on their specialties, and provides little incentive to bring different providers together for a holistic approach and coordinated care.
The ACA contains provisions for Medicare to test alternatives, such as value-based models, in which providers are paid based on patient health outcomes. The theory is to give providers financial incentives to help patients improve their health, reduce the impact of chronic diseases, and live healthier lives. Payments are based on the outcome of care, not on the number of visits or procedures completed. One Medicare program encourages the formation of accountable care organizations to treat patients more holistically and in better-coordinated fashion.
Other alternative approaches include capitation systems in which providers are paid a set amount per-person for caring for a population of patients (such as in some health maintenance organizations). And reference-based pricing has gained some traction in the state of Montana and elsewhere.
To our knowledge, no comprehensive assessment and comparison of these approaches has been made to date.
Confusion Around Medicare and Medicaid, Obamacare and the ACA
We don’t know the extent to which confusion around Medicare, Medicaid, Obamacare, and the ACA, created by misinformation and partisan disinformation, has affected the debate over how to best increase access to health insurance.
The Affordable Care Act and Obamacare both refer to the same legislation passed in 2010. Yet, a poll conducted 7 years after its passage found that more than a third of Americans (35%) did not understand that the ACA and Obamacare are the same thing.
The same poll revealed confusion over the relationship between Medicaid and the ACA. “Only 61% of adults knew that many people would lose coverage through Medicaid or subsidies for private health insurance if the ACA were repealed and no replacement enacted,” the researchers wrote.
This kind of confusion about government healthcare programs was particularly evident in the period when the ACA was being considered in Congress. Despite the fact that the ACA lowers the cost of Medicare, a federal government program, many people—including Medicare recipients—attended meetings sponsored by their members of Congress carrying signs that said: “Keep your government hands off my Medicare.”
What’s at Stake
Life Expectancy of the Uninsured
The high cost to society of providing healthcare is a common complaint, but there are high costs to not providing healthcare. Many studies have linked a lack of insurance to higher mortality rates and poorer health:
- A 2009 study in the American Journal of Public Health found that nationwide, 45,000 annual deaths were associated with a lack of health insurance. It found that uninsured, working-age Americans had a 40% higher risk of death than their privately insured counterparts.
- A 2017 meta-analysis of the literature published in the Annals of Internal Medicine found that being uninsured raised the risk of dying by more than 25%.
- A 2012 New England Journal of Medicine study that compared Medicaid expansion in three states compared with neighboring states found “a significant reduction in all-cause mortality” of 6.1% in the Medicaid-expansion states.
- Black women are more likely than White women to die from breast cancer. An American Cancer Society study found that differences in health insurance coverage—many more White women have insurance than Black women—explained about 35% of the excess risk of death in Black women.
Americans’ Personal Financial Health
Patients’ financial as well as physical wellbeing is at stake. “More than 13% of American adults—or about 34 million people—report knowing of at least one friend or family member in the past five years who died after not receiving needed medical treatment because they were unable to pay for it”, according to a study by Gallup and West Health.
The uninsured are particularly vulnerable. A 2016 survey by the Kaiser Family Foundation and the New York Times found that 53% of uninsured people reported problems paying household medical bills in the past year.
But roughly one in five people with insurance reported problems paying medical bills, as well.
Difficulty in paying medical bills can lead to bankruptcy. A survey of Americans who had declared bankruptcy found that 37% of them “very much agreed” that medical expenses contributed to their bankruptcy.
Some medical conditions can be so expensive that moderate-income patients are also vulnerable to the high costs of healthcare. A 2018 study in the American Journal of Medicine found that among the 9.5 million patients who were over 50 years old and diagnosed with cancer from 2000 to 2012, 42% had depleted all their assets after two years.
The Nation’s Financial Health
In an assessment of the nation’s post-pandemic fiscal health, the Governmental Accounting Office (GAO) first notes that “the federal government’s long-term fiscal path was unsustainable because debt was growing faster than the economy.” The GAO projects that the national debt will reach a historic high in 2028 and continue to grow faster than the economy.
According to both the GAO and the Congressional Budget Office (CBO), healthcare spending is the leading driver of long-term federal government spending. In its 2021 Long-Term Budget Outlook, the CBO projects government spending to average almost 30% of GDP between 2042-2051 – a 9% increase from the last decade, 2010-2019.
The primary contributor to the increase in healthcare spending is the continued rise in the cost of care, while our aging population is also a factor as it becomes an increasingly larger segment of the population.
The Committee for a Responsible Federal Budget wrote in 2018 that healthcare would consume a larger share of the federal budget over time. “In 1970, major health programs made up only 5% of the budget. That share increased to 20% by 2000 and 28% by 2017. By 2028, one-third of federal dollars not spent on interest will go toward health spending, and by 2040, nearly 40% will.”
Potential Obstacles
When President Lyndon Johnson proposed Medicare to provide medical coverage for the elderly in the 1960s, it was opposed by small-government conservatives, the American Medical Association (AMA), and others who called it socialized medicine.
Yet, Medicare quickly became so embedded in American society that it is considered an untouchable “third rail” that politicians dare not openly oppose. But the forces that opposed it then remain and resurface when healthcare reform is on the agenda.
Political Polarization
The Pew Research Center reports that a majority of Americans believe the federal government is responsible for making sure all Americans have healthcare coverage. However, examined more closely, there is a clear partisan bias in the results: 88% of Democrats say the federal government is responsible for making sure all Americans have healthcare coverage; 66% of Republicans say it isn’t.
The Affordable Care Act (ACA) is a clear example of this ideological divide. Throughout our history, Americans have tended to look to the federal government to address systemic problems like access to healthcare, and the ACA targets one specific aspect of the problem – uninsured and underinsured Americans. Democrats supported the ACA. Despite the fact that the ACA is based on free-market principles and is modeled on a conservative plan adopted in Massachusetts under a Republican governor, Republicans in the US Congress were united in opposing its passage and have persistently sought to undermine its effectiveness. And despite promises, no equally effective Republican alternative has yet been proposed.
This failure to offer viable alternatives leaves open the question: If the federal government is not allowed to solve the problem, what organization or group is in a position to do so?
Industry Opposition
Typically, proposed reforms that threaten healthcare industry interests provoke fierce opposition.
Last year, the pharmaceutical sector alone spent more on lobbying than any other industry. Hospitals and professional organizations are also big spenders. There were eight lobbyists for each member of Congress working to influence health reform bills in 2009. In the end, the American Medical Association successfully lobbied to have the following provisions removed from the ACA:
- $300 yearly fee for doctors who participate in Medicare or Medicaid
- tax on cosmetic surgery
- 5% Medicare payment cuts to the top 10% of Medicare billers
Today, the Partnership for America’s Health Care Future, a lobbying group founded by organizations including the Blue Cross Blue Shield Association and the AMA (which has since exited), are fighting Medicare For All.
Lack of Contact with the Medical System
About 80% of healthcare dollars are spent on about 20% of the population.
In any given year, most people will not need anything but the most basic healthcare, meaning that a majority of people avoid significant interaction with the healthcare system. Only a minority will need urgent, expensive, or hard-to-access care. As a result, there is limited political pressure to fix urgent problems.
“That really has been working in favor of the status quo,” explains Simon F. Haeder, a healthcare policy expert and assistant professor at Penn State University. “If we all experienced how shady the system is in any given year, then we’d all ask for a lot of changes.”
In an effort to improve health outcomes, Lisa Fitzpatrick, M.D., started a health information company that uses storytelling, videos, social media and on-the-street person-to-person conversations to increase trust in the medical establishment among low income communities.
Additional Considerations
National Debt
Already high before the pandemic, the debt has now reached levels not seen since World War II. Healthcare spending is one of the biggest drivers of federal spending. Further increases in the national debt may threaten future investment in government solutions to healthcare access.
Public Health Preparedness
The pandemic exposed weaknesses in healthcare systems around the world, and the US was no exception. Black, Latino, and Native Americans were more likely to contract, be hospitalized with, and die of COVID-19, revealing the inequities of healthcare access in this country. One uninsured patient received a $34,927.43 bill for her COVID-19 treatment.
Infrastructure
Proposals for improving the healthcare infrastructure, including increasing the reach of high speed internet in rural and low-income communities, can strengthen at-risk populations’ contact with the healthcare system. Telehealth is one clear way to deliver care to medical deserts and at the same time reduce overall costs of care. Without high speed internet in those communities, however, telehealth will not close gaps in care.
Immigration
When estimating the cost of potential government-driven solutions, it will be necessary to define what coverage applies to immigrants, and to understand how many immigrants will be accepted into the country and made eligible on an annual basis. The rate at which new immigrants will be permitted to enter the country, then, is needed for accurate preparation and budgeting of healthcare resources.
Frequently Asked Questions
Did expanded insurance coverage increase wait times?
Is healthcare a human right?
In The Wealth of Nations, published in 1776, Adam Smith wrote that a nation cannot truly flourish if a sizable number of its people are “poor and miserable.” In discussing the virtues of the increasing division of labor and the inequities it produced, he argued, “It is but equity, besides, that they who feed, clothe, and lodge the whole body of the people, should have such a share of the produce of their own labour as to be themselves tolerably well fed, clothed, and lodged.”
Since it is the division of labor that has given those trained in medicine the opportunity to advance our knowledge and technology for treating illnesses and extending life, would Smith’s vision include access to healthcare as a matter of equity for all?
The United Nations Universal Declaration of Human Rights, which the US helped draft, seems to think so. It states, “Everyone has the right to a standard of living adequate for the health and well-being of himself and of his family, including food, clothing, housing and medical care ….”
Not everyone agrees. One physician, Philip Barlow, has argued that it is unproductive to consider healthcare a right. After all, healthcare is difficult to define. While we might agree that it should include life-saving heart surgery and organ transplantation, might there be less agreement around cosmetic surgery or erectile dysfunction? Barlow raises similar questions in an editorial in the British Medical Journal.
Did expanded insurance coverage increase wait times?
When the ACA passed, some feared the medical infrastructure would not be able to absorb the influx of new patients.
Although the ACA greatly increased the number of people with insurance, especially through Medicaid, “findings on expansion’s effect on provider capacity are mixed, with studies showing increases, decreases, or no effects on measures like appointment availability or wait times”, according to a report by Kaiser Health News.
Whether continued expansion could be a problem in the future is an open question. There are already waiting times to see specialists in many parts of the country and for many conditions. Many workforce studies predict shortages of physicians in both primary care and specialties in coming years.
Is defensive medicine driving up healthcare costs?
Defensive medicine is the term for practicing medicine with an eye toward avoiding a malpractice lawsuit. Physicians may go beyond what is required to diagnose and treat the patient to ensure they are not missing any possible condition.
American healthcare providers run many more diagnostic tests than in similar Western countries, for example. It is not known how much of this testing is due to defensive medicine, payment incentives, patient demands, or other factors, however.
One study found that physicians practicing in a system in which they do not need to worry about liability lowered hospital inpatient spending by 5%.
A 2016 legislative analysis by the Congressional Budget Office of a proposed federal law to limit malpractice lawsuits estimated it would reduce overall healthcare spending by one half of one percent (0.5%).
Overall, there is little evidence that proposed reforms to counter the costs of defensive medicine are likely to have much effect on overall costs.
Do high deductible plans discourage excess care?
There have been many proposals to shape insurance policies in ways that encourage lower spending by patients. One such proposal encourages implementing high-deductible insurance policies to deter patients from seeking excessive care. If patients have to pay out-of-pocket to see a doctor, it assumes, for example, they may be more likely to rest at home with the common cold instead of seeking treatment.
Of course, a counter-argument is that high-deductible plans discourage preventive care, i.e. cheaper intervention before a problem grows. In this scenario, a high deductible plan may, in the long run, cost more.
Tools & Resources
General Information
The Commonwealth Fund publishes a wealth of healthcare research, as does The Kaiser Family Foundation (KFF). The Pew Research Center conducts survey research on a range of topics, including Americans’ attitudes about healthcare.
Government and Politics
Business influence. Open Secrets publishes details on spending by the healthcare industry on lobbying, federal campaigns, and political parties in the US.
COVID spending. The US government has approved trillions of dollars in spending on the healthcare system to address the COVID-19 crisis. Find out more with the Committee for a Responsible Budget’s COVID Money Tracker.
Where your taxes go. See how much of your federal taxes go to healthcare with the National Priorities Project Tax Receipt.
Making Healthcare More Affordable
Price transparency. ClearHealthCosts has been collecting cost data on medical services since 2010 so that patients can find the most affordable care available in the city where they live. Founded by Jeanne Pinder, a former NY Times journalist.
Financial aid. Advocatia helps hospitals connect low-income patients with financial aid programs that can help reduce their costs of care. Started by Ryan Brebner, who founded the company with his sister to make better use of available aid programs.
Sources
The URLs included with the sources below were good links when we published. However, as third party websites are updated over time, some links may be broken. We do not update these broken links. If you are interested in the source, it may be possible to find it by copying and pasting the URL into a search on the Internet Archive Wayback Machine. From the search results, be sure to choose a date from around the time our article was published.
Key Takeaways
Max Roser, “Why is life expectancy in the US lower than in other rich countries?”, Our World in Data, Oct 29, 2020, https://ourworldindata.org/us-life-expectancy-low, accessed May 21, 2021
Credit Suisse, “Global wealth report”, Oct 2020, https://www.credit-suisse.com/about-us/en/reports-research/global-wealth-report.html, accessed Apr 9, 2021
Kenneth D. Kochanek, M.A., Robert N. Anderson, Ph.D., and Elizabeth Arias, Ph.D., “Changes in life expectancy at birth 2010-2018”, CDC, Jan 2020, https://www.cdc.gov/nchs/data/hestat/life-expectancy/lifeexpectancy-H.pdf, accessed Apr 9, 2021
Papanicolas, L.R. Woskie, A.K. Jha, “Health care spending in the United States and other high-income countries”, JAMA, Mar 13, 2018, 1024-1039, https://www.ncbi.nlm.nih.gov/pubmed/29536101, synopsis: https://www.commonwealthfund.org/publications/journal-article/2018/mar/health-care-spending-united-states-and-other-high-income, accessed Feb 25, 2020
Rabah Kamal, Giorlando Ramirez, and Cynthia Cox, “How does health spending in the US compare to other countries?”, Health System Tracker, Dec 23, 2020, https://www.healthsystemtracker.org/chart-collection/health-spending-u-s-compare-countries/#item-spendingcomparison_gdp-per-capita-and-health-consumption-spending-per-capita-2019, accessed Mar 24, 2021
Eli Saslow, “‘Out here, it’s just me’: In the medical desert of rural America, one doctor for 11,000 square miles”, Washington Post, Sep 29, 2019, https://www.washingtonpost.com/national/out-here-its-just-me/2019/09/28/fa1df9b6-deef-11e9-be96-6adb81821e90_story.html, accessed Feb 24, 2020
Simon F. Haeder, “US health care system: A patchwork that no one likes”, The Conversation, Oct 18, 2017, https://theconversation.com/us-health-care-system-a-patchwork-that-no-one-likes-85252, accessed Apr 8, 2021
Patrick G. Lee, “Who Makes Sure Hospital Mergers Do No Harm? Almost Nobody.”, ProPublica, Jun 9, 2016, https://www.propublica.org/article/who-makes-sure-hospital-mergers-do-no-harm-almost-nobody, accessed Apr 8, 2021
Joe Eaton and M.B. Pell, “Lobbyists swarm Capitol to influence health reform”, Center for Public Integrity, May 19, 2014, https://publicintegrity.org/health/lobbyists-swarm-capitol-to-influence-health-reform/, accessed Mar 24, 2021
Problem Definition
Advisory Board, “Who’s underinsured in America, in 4 charts”, Feb 8, 2019, https://www.advisory.com/en/daily-briefing/2019/02/08/underinsured, accessed May 18, 2021
Problem Scope
Robin A. Cohen, Michael E. Martinez, Brian W. Ward, “Health insurance coverage: Early release of estimates from the National Health Interview Survey, 2009”, National Center for Health Statistics, Jun 2010, https://www.cdc.gov/nchs/data/nhis/earlyrelease/insur201006.htm, accessed Apr 1, 2020
Edward R. Berchick, Jessica C. Barnett, And Rachel D. Upton, Health Insurance Coverage in the United States: 2018, US Census Bureau, Nov 2019, https://www.census.gov/content/dam/Census/library/publications/2019/demo/p60-267.pdf, accessed Apr 2, 2020
“US health insurance coverage in 2020: A looming crisis in affordability”, The Commonwealth Fund, Aug 19, 2020, https://www.commonwealthfund.org/publications/issue-briefs/2020/aug/looming-crisis-health-coverage-2020-biennial, accessed Mar 24, 2021
Lydia Saad, “More Americans Delaying Medical Treatment Due to Cost”, Gallup, Dec 9, 2019, https://news.gallup.com/poll/269138/americans-delaying-medical-treatment-due-cost.aspx, accessed Apr 2, 2020
American Cancer Society, “Medical costs create hardships for more than half of Americans: 137 million adults in the United States suffered medical financial hardship in 2015/2017”, Science Daily, May 2,2019, https://www.sciencedaily.com/releases/2019/05/190502100818.htm, accessed Apr 2, 2020
Centers for Medicare and Medicaid Services, “Historical”, Last modified Dec 17, 2019, https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/NationalHealthAccountsHistorical, accessed Feb 25, 2020
Susan L. Hayes, Sara R. Collins, David C. Radley, “How Much U.S. Households with Employer Insurance Spend on Premiums and Out-of-Pocket Costs: A State-by-State Look”, The Commonwealth Fund, May 23, 2019, https://www.commonwealthfund.org/publications/issue-briefs/2019/may/how-much-us-households-employer-insurance-spend-premiums-out-of-pocket, accessed Apr 8, 2020
Rabah Kamal, Giorlando Ramirez, Cynthia Cox, “How does health spending in the U.S. compare to other countries?”, Peterson-KFF, Dec 23, 2020, https://www.healthsystemtracker.org/chart-collection/health-spending-u-s-compare-countries/#item-spendingcomparison_health-consumption-expenditures-per-capita-2019, accessed May 18, 2021
Consensus study report, “U.S. health in international perspective: shorter lives, poorer health”, National Academies Press, 2013, https://www.nap.edu/catalog/13497/us-health-in-international-perspective-shorter-lives-poorer-health, press release: http://www8.nationalacademies.org/onpinews/newsitem.aspx?RecordID=13497, accessed Feb 25, 2020
Papanicolas, L.R. Woskie, A.K. Jha, “Health care spending in the United States and other high-income countries”, JAMA, Mar 13, 2018, 1024-1039, https://www.ncbi.nlm.nih.gov/pubmed/29536101, synopsis: https://www.commonwealthfund.org/publications/journal-article/2018/mar/health-care-spending-united-states-and-other-high-income, accessed Feb 25, 2020
Diane Archer, “Medicare is more efficient than private insurance”, Health Affairs, Sep 20, 2011, https://www.healthaffairs.org/do/10.1377/hblog20110920.013390/full/, accessed Feb 25, 2020
Pew Charitable Trusts, “Payment policies to manage pharmaceutical costs”, Mar 16, 2017, https://www.pewtrusts.org/en/research-and-analysis/reports/2017/03/payment-policies-to-manage-pharmaceutical-costs, accessed Feb 26, 2020
Alisa Tank, “Physician salary report 2020: Salaries rising prior to COVID-19 impacts”, Weatherby Healthcare, Jun 17, 2020, https://weatherbyhealthcare.com/blog/annual-physician-salary-report, accessed May 18, 2021
Emily Rappleye, “4 trends in physician pay”, Beckers Hospital Review, Dec 5, 2019, https://www.beckershospitalreview.com/compensation-issues/4-trends-in-physician-pay.html, accessed May 18, 2021
Greg Rosalsky, “Are Doctors Overpaid?”, NPR/Planet Money, Mar 12, 2019, https://www.npr.org/sections/money/2019/03/12/702500408/are-doctors-overpaid, accessed May 18, 2021
Reed Abelson, “When hospitals merge to save money, patients often pay more”, New York Times, Nov 14, 2018, https://www.nytimes.com/2018/11/14/health/hospital-mergers-health-care-spending.html, accessed Feb 25, 2020
Diane Archer, “No Competition: The Price Of A Highly Concentrated Health Care Market”, Health Affairs, Mar 6, 2013, https://www.healthaffairs.org/do/10.1377/hblog20130306.028873/full/, accessed May 18, 2021
Phil Galewitz, “The startlingly high cost of the ‘free’ flu shot”, Kaiser Health News, Nov 19, 2019, https://khn.org/news/the-startlingly-high-cost-of-the-free-flu-shot/, accessed Feb 25, 2020
Robert M. Pearle, MD, “Are You A Patient Or A Healthcare Consumer?”, Forbes, Oct 15, 2015, https://www.forbes.com/sites/robertpearl/2015/10/15/are-you-a-patient-or-a-health-care-consumer-why-it-matters/?sh=72c3d02f2b4d, accessed May 26, 2021
JK Wall, “Think Again: Health Insurers Have No Reason To Reduce the Price of Health Care”, The Health Care Blog, Jan 1, 2016, https://thehealthcareblog.com/blog/2016/01/01/think-again-health-insurers-have-no-reason-to-reduce-the-price-of-health-care/, accessed May 19, 2021
Marshall Allen, “Why Your Health Insurer Doesn’t Care About Your Big Bills”, NPR, May 25, 2018, https://www.npr.org/sections/health-shots/2018/05/25/613685732/why-your-health-insurer-doesnt-care-about-your-big-bills, accessed May 19. 2021
Johanna Butler, “Independent Analysis Finds Montana Has Saved Millions by Moving Hospital Rate Negotiations to Reference-Based Pricing”, National Academy for State Health Policy, Apr 5, 2021, https://www.nashp.org/new-analysis-finds-montana-has-saved-millions-by-moving-hospital-rate-negotiations-to-reference-based-pricing/, accessed May 19, 2021
Eli Saslow, “‘Out here, it’s just me’: In the medical desert of rural America, one doctor for 11,000 square miles”, Washington Post, Sep 29, 2019, https://www.washingtonpost.com/national/out-here-its-just-me/2019/09/28/fa1df9b6-deef-11e9-be96-6adb81821e90_story.html, accessed Feb 24, 2020
American Hospital Association, “AHA Rural Report: challenges facing rural communities and the roadmap to ensure local access to high-quality, affordable care”, page 5, https://www.aha.org/system/files/2019-02/rural-report-2019.pdf, accessed Feb 24, 2020
L Skinner, DO Staiger, DI Auerbach, PI Buerhaus, “Implications of an aging rural physician workforce”, New England Journal of Medicine, July 25, 2019, 299-301, https://www.ncbi.nlm.nih.gov/pubmed/31340091, accessed Feb 24, 2020
Michael Braga, Jennifer F. A. Borresen, Dak Le, Jonathan Riley, “‘Leaving billions of dollars on the table,’ rural hospitals foundering in states that declined Obamacare”, GateHouse Media, USA Today Network News, Jul 28, 2019, https://gatehousenews.com/ruralhospitals/financialtroubles/, accessed Feb 24, 2020
Karen E. Joynt, Nguyen Nguyen, Lok Wong Samson, and John E. Snyder, (ASPE) with Amanda Lechner and Omotomike Ogunwumiju (Mathematica Policy Research), “Rural hospital participation and performance in value-based purchasing and other delivery system reform initiatives”, ASPE Issue Brief, US Department of Health and Human Services, Assistant Secretary for Planning and Evaluation, Oct 19, 2016, https://aspe.hhs.gov/pdf-report/rural-hospital-participation-and-performance-value-based-purchasing-and-other-delivery-system-reform-initiatives, accessed Feb 24, 2020
Michael Braga, Jennifer F. A. Borresen, Dak Le and Jonathan Riley, “Rural hospitals foundering in states that declined Obamacare”, Gatehouse Media/USA Today, Jul 28, 2019, https://stories.usatodaynetwork.com/ruralhospitals/financialtroubles/, accessed Apr 2, 2020
Kaiser Family Foundation, “Status of State Action on the Medicaid Expansion Decision”, May 19, 2021, https://www.kff.org/health-reform/state-indicator/state-activity-around-expanding-medicaid-under-the-affordable-care-act/?activeTab=map¤tTimeframe=0&selectedDistributions=status-of-medicaid-expansion-decision&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D, accessed May 19, 2021
American Association of Medical Colleges, “New findings confirm predictions on physician shortage”, Apr 23, 2019, https://www.aamc.org/news-insights/press-releases/new-findings-confirm-predictions-physician-shortage, accessed Feb 26, 2020
Limits to What We Know
Adam Smith, The Wealth of Nations, Amazon Kindle, loc 1278
UN Universal Declaration of Human Rights, Dec 10, 1948, https://www.un.org/en/about-us/universal-declaration-of-human-rights, accessed May 27, 2021
Larisa Antonisse, Rachel Garfield, Robin Rudowitz, Madeline Guth, “The effects of Medicaid expansion under the ACA: updated findings from a literature review”, Kaiser Family Foundation, Aug 15, 2019, https://www.kff.org/medicaid/issue-brief/the-effects-of-medicaid-expansion-under-the-aca-updated-findings-from-a-literature-review-august-2019/, accessed Feb 25, 2020
Kyle Dropp, Brendan Nyban, “One-third don’t know Obamacare and Affordable Care Act are the same”, New York Times, Feb 7, 2017, https://www.nytimes.com/2017/02/07/upshot/one-third-dont-know-obamacare-and-affordable-care-act-are-the-same.html, accessed Mar 15, 2020
Juliette Cubanski, Tricia Neuman, Gretchen Jacobson, Cristina Boccuti, “What Are the Implications of Repealing the Affordable Care Act for Medicare Spending and Beneficiaries?” KFF, Dec 13, 2016, https://www.kff.org/health-reform/issue-brief/what-are-the-implications-of-repealing-the-affordable-care-act-for-medicare-spending-and-beneficiaries/, accessed May 27, 2021
Bob Cesca, “Keep your goddamn government hands off my Medicare!” HuffPost, Sep 5, 2009, updated Dec 6, 2017, https://www.huffpost.com/entry/get-your-goddamn-governme_b_252326, accessed Mar 15, 2020
Timothy Noah, “The Medicare-isn’t-government meme”, Slate.com, Aug 5, 2009, https://slate.com/news-and-politics/2009/08/help-slate-track-the-medicare-isn-t-government-meme.html, accessed Mar 15, 2020
Margot Sanger-Katz, “They want it to be secret: how a common blood test can cost $11 or almost $1,000”, New York Times, Apr 30, 2019, https://www.nytimes.com/2019/04/30/upshot/health-care-huge-price-discrepancies.html, accessed Feb 25, 2020
Steven Brill, “Bitter pill: why medical bills are killing us”, Time, Apr 4, 2013, https://time.com/198/bitter-pill-why-medical-bills-are-killing-us/, accessed Feb 25, 2020
Steffie Woolhandler, David U. Himmelstein, “The relationship of health insurance and mortality: is lack of insurance deadly?”, Annals of Internal Medicine, Sep 19, 2017, https://annals.org/aim/fullarticle/2635326/relationship-health-insurance-mortality-lack-insurance-deadly, accessed Feb 24, 2020
What is at Stake?
David Cecere, “New study finds 45,000 deaths annually linked to lack of health coverage”, Harvard Gazette, Sep 17, 2009, https://news.harvard.edu/gazette/story/2009/09/new-study-finds-45000-deaths-annually-linked-to-lack-of-health-coverage, accessed Feb 24, 2020
Benjamin D. Sommers, Katherine Baicker, Arnold M. Epstein, “Mortality and access to care among adults after state Medicaid expansions”, New England Journal of Medicine, Sep 2012, 1025-34, https://www.ncbi.nlm.nih.gov/pubmed/22830435, accessed Feb 24, 2020
Sandy McDowell, “Study: lack of insurance linked to higher breast cancer death rates in black women”, American Cancer Society, Oct 16, 2017, https://www.cancer.org/latest-news/study-lack-of-insurance-linked-to-higher-breast-cancer-death-rates-in-black-women.html, accessed Feb 24, 2020
Dan Witters, “Millions in U.S. lost someone who couldn’t afford treatment”, Gallup, Nov 12, 2019, https://news.gallup.com/poll/268094/millions-lost-someone-couldn-afford-treatment.aspx, accessed Feb 25, 2020
Liz Hamel, Mira Norton, Karen Pollitz, Larry Levitt, Gary Claxton, Mollyann Brodie, “The burden of medical debt: results from the Kaiser Family Foundation/New York Times medical bills survey”, Jan 2016, https://www.kff.org/wp-content/uploads/2016/01/8806-the-burden-of-medical-debt-results-from-the-kaiser-family-foundation-new-york-times-medical-bills-survey.pdf, accessed Feb 24, 2020
Steffie Woolhandler, David U. Himmelstein, “Medical bankruptcy: still common despite the Affordable Care Act”, American Journal of Public Health, March 2019, http://www.pnhp.org/docs/AJPHBankruptcy2019.pdf, accessed Feb 24, 2020
A.M. Gilligan, D.S. Alberts, D.J. Roe, G.H. Skrepnek, “Death or debt? National estimates of financial toxicity in persons with newly-diagnosed cancer”, American Journal of Medicine, Oct 2018, 1187-99, https://www.amjmed.com/article/S0002-9343(18)30509-6/fulltext, accessed Feb 25, 2020
Government Accounting Office, “The Nation’s Fiscal Health: After Pandemic Recovery, Focus Needed on Achieving Long-Term Fiscal Sustainability”, Mar 23, 2021, https://www.gao.gov/products/gao-21-275sp, accessed May 20, 2021
Congressional Budget Office, “The 2021 Long-Term Budget Outlook”, Mar 2021, https://www.cbo.gov/publication/57038, accessed May 20, 2021
Committee for a Responsible Federal Budget, “American health care: health spending and the federal budget”, May 16, 2018, https://www.crfb.org/papers/american-health-care-health-spending-and-federal-budget, accessed Feb 25, 2020
Potential Obstacles
Bradley Jones, “Increasing share of Americans favor a single government program to provide health care coverage”, Pew Research Center, Sep 29, 2020, https://www.pewresearch.org/fact-tank/2020/09/29/increasing-share-of-americans-favor-a-single-government-program-to-provide-health-care-coverage/, accessed Mar 24, 2021
Bill Adair and Angie Drobnic Holan, “PolitiFact’s Lie of the Year: ‘A government takeover of health care’”, PolitiFact, Dec 16, 2010, https://www.politifact.com/article/2010/dec/16/lie-year-government-takeover-health-care/, accessed Mar 30, 2021
Open Secrets, “Industries”, https://www.opensecrets.org/federal-lobbying/industries?cycle=a, accessed Mar 29, 2021
Adam Cancryn, “The army built to fight ‘Medicare For All’”, Politico, Nov 25, 2019, https://www.politico.com/news/agenda/2019/11/25/medicare-for-all-lobbying-072110, accessed Mar 25, 2021
Ian K. Kullgren, “Does 20% of the population really use 80% of health care dollars?”, PolitiFact, Feb 23, 2012, https://www.politifact.com/factchecks/2012/feb/23/alan-bates/does-20-percent-population-really-use-80-health-ca/, accessed Mar 30, 2021
Dr. Simon Haeder, interview with Ciara McLaren, Mar 30, 2021
Key Considerations
Congressional Budget Office, “An Update to the Budget Outlook: 2020 to 2030”, Oct 6, 2020, https://www.cbo.gov/system/files/2020-09/56517-Budget-Outlook.pdf, accessed Mar 30, 2021
Abigail Abrams, “Total cost of her COVID-19 treatment: $34,927.43”, TIME, Mar 19, 2020, https://time.com/5806312/coronavirus-treatment-cost/, accessed Mar 30, 2021
CDC, “Risk for COVID-19 infection, hospitalization, and death by race/ethnicity”, Mar 12, 2021, https://www.cdc.gov/coronavirus/2019-ncov/covid-data/investigations-discovery/hospitalization-death-by-race-ethnicity.html, accessed Mar 30, 2021
FAQs
Larisa Antonisse, Rachel Garfield, Robin Rudowitz, Madeline Guth, “The effects of Medicaid expansion under the ACA: updated findings from a literature review”, Kaiser Family Foundation, Aug 15, 2019, https://www.kff.org/medicaid/issue-brief/the-effects-of-medicaid-expansion-under-the-aca-updated-findings-from-a-literature-review-august-2019/, accessed Feb 25, 2020
American Association of Medical Colleges, “New findings confirm predictions on physician shortage”, Apr 23, 2019, https://www.aamc.org/news-insights/press-releases/new-findings-confirm-predictions-physician-shortage, accessed Feb 26, 2020
Peter O’Dowd, “Rural hospitals say ‘Medicare for all’ would end up ‘closing our doors’”, Here and Now, WBUR radio, Aug 16, 2019, https://www.wbur.org/hereandnow/2019/08/16/rural-hospitals-medicare-for-all-health-care, accessed Feb 25, 2020
Chapin White, “Contrary to cost-shift theory, lower Medicare hospital payment rates for inpatient care lead to lower private payment rates”, Health Affairs, May 2013, https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2012.0332, accessed Feb. 25, 2020
Austin Frakt, “JAMA Forum: hospitals don’t shift costs from Medicare or Medicaid to private insurers”, JAMA, Jan 4, 2017, https://newsatjama.jama.com/2017/01/04/jama-forum-hospitals-dont-shift-costs-from-medicare-or-medicaid-to-private-insurers/, accessed Feb 25, 2020
Michael D. Frakes, Jonathan Gruber, “Defensive medicine: evidence from military immunity”, NBER Working Paper No. 24846, National Bureau of Economic Research, Jul 2018, https://www.nber.org/papers/w24846, accessed Feb 26, 2020
Congressional Budget Office, “Limit medical malpractice claims”, Dec 8, 2016, https://www.cbo.gov/budget-options/2016/52241, accessed Feb 26, 2020
Rajender Agarwal, Olena Mazurenko, and Nir Menachemi, “High-deductible health care plans reduce health care cost and utilization, including use of needed preventive services”, Health Affairs, Oct 2017, https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2017.0610, accessed Apr 1, 2021
Credits
Authors: Eric Seaborg, Ciara McLaren, George Linzer
Published: May 27, 2021
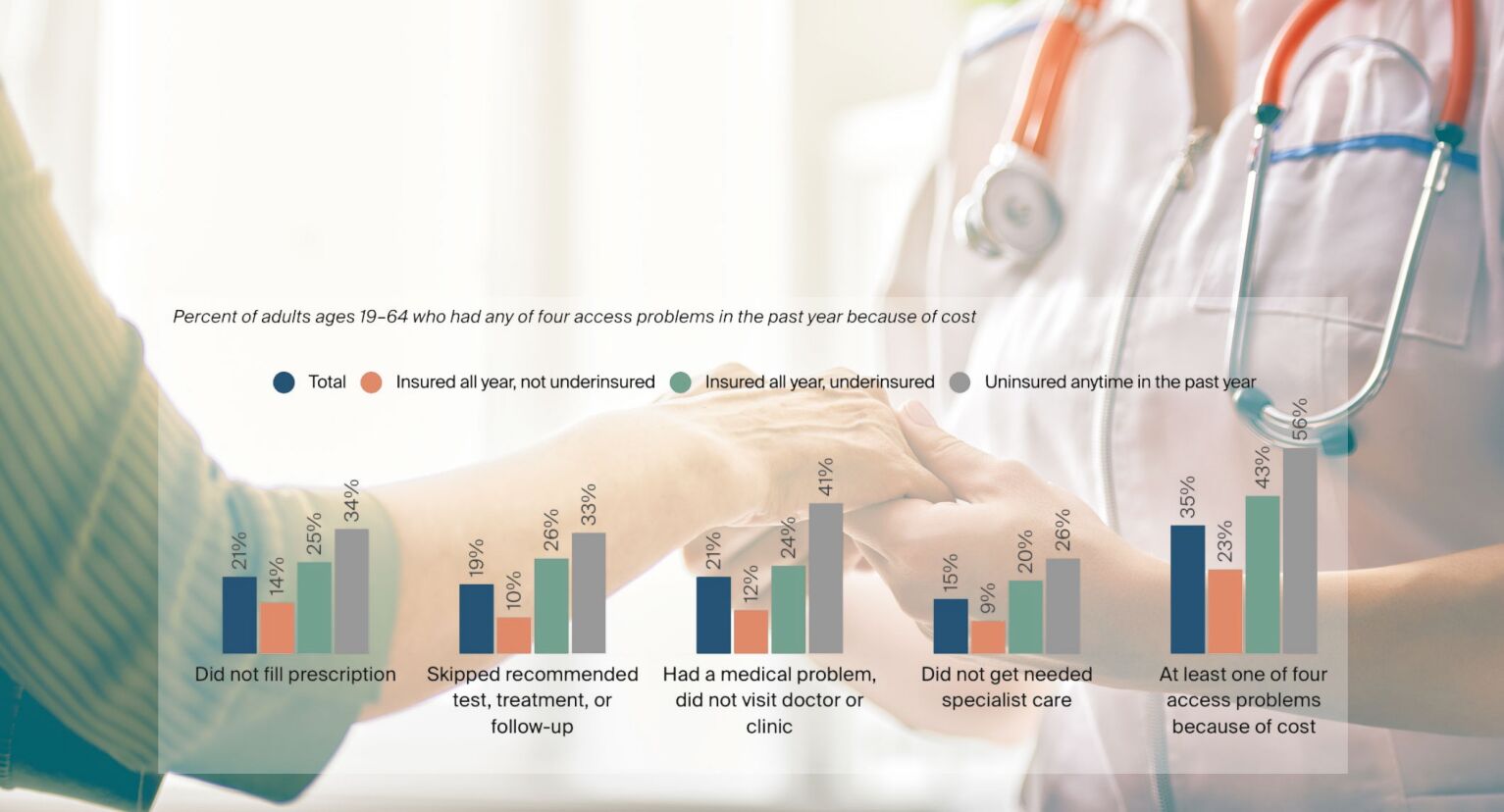
Feature image: George Linzer, based on work by Choreograph and Commonwealth Fund